Invasion of the Microbes
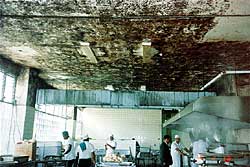
Since the beginning of the 1980s, and arguably earlier, the term "Sick Building Syndrome" was coined to describe a series of sometimes-mysterious ailments claimed by occupants of certain buildings. Let's begin by recognizing that the very term "Sick Building Syndrome" is somewhat of a misnomer in that it implies a defined set of problems with a specific set of symptoms.
In our experience, building design, operation and maintenance problems run in a continuum from major life-threatening malfunctions to trivial or non-existent issues. Even minor problems -- sometimes perceived as very serious -- cause stress to building occupants unless there is a timely, competent response by building managers. If, however, the causative agent is biological matter growing in some component of the building mechanical system, how is a building manager expected to diagnose this? The manager of the Bellevue-Stratford Hotel in Philadelphia surely asked himself this question after the world's first catastrophic outbreak of Legionnaires disease struck his property in late July of 1976, eventually claiming the lives of 34 guests and sickening a further 221.
Relatively little is known about the part played by microbes in causing ailments associated with buildings, but there are some things we can do to discourage their presence in building heating, ventilating and air-conditioning (HVAC) systems. We must begin by knowing the basic forms these organisms take.
In indoor air quality studies of more than 2,500 building over the past two decades, we have found fungal growth to be the single most problematic contaminant. |
Viruses
Viruses are the smallest organisms of concern. Because they are incapable of producing their own enzymes for nutrition/reproduction, they are generally only considered to be able to survive within living cells. For this reason there is little opportunity for air conditioning systems to play a large role in their proliferation. That said, infectious droplet transmission in poorly ventilated spaces might be a common way for viruses to spread, especially when protected inside other particles or cells long enough to survive in the circulating air.
Bacteria
Bacteria are too small to be seen with the naked eye, however, when cultured artificially they readily form colonies of millions of single cells that are easily visible. A general way to define organisms as bacterial is the lack of a membrane separating the nuclear material from the rest of the cell components. The most common bacteria found within building HVAC systems are relatively harmless and are equally likely to be found all over your desk - they frequently include members of the genera Bacillus and Micrococcus as well as diptheroid bacillus.
Some potentially harmful bacterial organisms include Pseudomonas sp., Flavobacterium, Staphylococcus Pyrogenes and of course Legionella pneumophila, of which more than 13 serotypes have now been identified. This includes the organism that causes Pontiac Fever, after an early definitive outbreak occurred in Pontiac, Mich. in 1969. The Legionella bacterium favors stagnant water in the temperature range of 70 to 115 degrees Fahrenheit and is sometimes found in cooling towers, rarely used showerheads and drinking water stations. Older "tepid" water supply systems are also common breeding grounds for this organism. Sound hygienic water maintenance practices and use of appropriate biocidal treatments especially in cooling towers has proven to be an effective tool in controlling this organism.
Fungi
Fungi, yeasts and molds are generally more complex structures than bacteria and exist as single or multi-cell or filamentous organisms. They reproduce sexually or asexually sometimes producing large numbers of spores that can be carried in air streams. The most common genera, found to be widespread throughout the world both indoors, inside HVAC systems and in the outdoors, are Cladosporium, Alternaria, Penicillium and Aspergillus. These four genera are also found to be the most prevalent in causing allergic respiratory disease. In particular the two species Aspergillus Niger and Fumigatus can cause potentially serious lung infections.
Thankfully less common, but equally serious health impacts are created by Stachybotrys sp. This organism favors cellulose media such as paper or cardboard, and relatively wet conditions for optimum growth. In indoor air quality studies of more than 2,500 buildings over the past two decades, we have found fungal growth to be the single most problematic contaminant, more so than bacteria, dust, carbon monoxide or a host of other indoor air constituents.
Protozoans
These organisms are generally more advanced and complex. They are able to colonize swamp cooler reservoirs and improperly draining condensate trays. Aerosolization of their cells occurs directly from the contaminated water, or from the residue as the water evaporates. These organisms can cause ailments such as hypersensitivity, pneumonitis, humidifier fever, asthma and allergic rhinitis.
No formal standards for indoor air microbial levels exists but, however, based on hospital operating room and other building experience, we feel that no more than 750 colony forming units per cubic meter of air should be present in office buildings. |
Again, good hygienic practices in condensate trays and other locations where water is stored best prevents proliferation of their numbers. We routinely recommend to our clients that they use biocidal chemical packs in condensate trays to encourage proper drainage and prevent growth of these organisms. Care must be taken with product selection however, in order to ensure the packs do not expire prematurely and their wrappers do not clog the drains.
Sources
Microbes gain entry into building systems in many ways, including via construction dust and debris, dirt drawn in via the outside air intakes, and via the return systems from building occupants and indoor activities. For instance, it has been calculated that each human sheds about seven million particles and cells per minute, and each of these carries with it an average of four microbial cells. As a result, there is always some background level of microbiological activity in HVAC systems. If the supply and return system is heavily loaded with dirt, this provides nutrition for microbial growth. Any condensation or other free water may allow for a healthy colony to quickly spread across a surface -- and particularly prone to this is internal fibrous glass insulation, especially where it has become wet from carry over from cooling coils or condensate trays.
Sampling
Sampling for microbes must be done with care if the results are not to be misleading. For instance, there is little or no point in sampling for Legionella bacteria in indoor air as this could result in a false negative -- the place to sample for this organism is in the water supply at source. Similarly, the absence of a positive result in an air sample for Stachybotrys sp. should not be taken to mean no problem exists if the black, slightly slimy colonies are visible on building substrates. Even if these colonies are currently absent but wet, humid growth conditions exist on say, paper-coated gypsum wallboard, corrective action should be taken immediately. That is not to say that air sampling is of no use. Careful air sampling, with controls taken in outdoor air, can be very helpful in determining if the interior of the building is unusually heavily infested with both bacterial and fungal organisms. If the numbers and types of species present are very different than found in outdoor air,
this should be cause for concern. If there are very high numbers of common bacteria present indoors, especially compared with outdoors, but few fungal numbers, this is often a sign that the building is simply poorly ventilated.
VOC sampling may prove useful in tracking down mold hidden in walls, thereby eliminating the need for wholesale destructive testing. |
There are currently no "official" standards for levels of bacteria and fungi either on surfaces in HVAC systems or building surfaces in general and our results are interpreted based on field experience. Likewise, no formal standards for indoor air microbial levels exists but, based on hospital operating room and other building experience and we feel that no more than 750 colony forming units per cubic meter of air should be present in office buildings. However, such a standard is essentially an arbitrary one and results are interpreted based on field experience and comparison with outdoor air levels of bacteria and fungi on the day of testing.
Conclusions
There is still much to learn about the means by which microorganisms flourish in buildings, and their relationships to the humans that occupy them. Research is ongoing on dose-response relationships, and the role of microbial by-products such as bacterial endotoxins and fungal glucans on symptomatology. We are currently evaluating the use of volatile organic compound (VOC) sampling for specific VOCs produced by fungal growth. This technique may prove useful in tracking down mold hidden in walls, thereby eliminating the need for wholesale destructive testing. It may also be that "new" microbes emerge that prove to play a part in building related illnesses in the same way that L. pneumophila emerged. It is inevitable, however, that we will continue to compete with microbes for our living and working space -- as building technologies change we can be sure that they will find ways to adapt and thrive in new kinds of environments.
This article originally appeared in the June 2001 issue of Environmental Protection, Vol. 12, No. 6, p. 68.
This article originally appeared in the 06/01/2001 issue of Environmental Protection.
About the Author
Dr. Robin Autenrieth is a professor in the Department of Civil Engineering at Texas A&M University. She is also president of the Association of Environmental Engineering & Science Professors (AEESP).